IN A NUTSHELL
Who’s the villain in nutritional rickets?
Nutritional rickets is not an uncommon condition in infancy and childhood, but is often missed as it initially presents with comorbidities such as pneumonia or dilated cardiomyopathy secondary to hypocalcaemia. Vitamin D deficiency has for many years been thought to be the major role player in the pathogenesis of nutritional rickets. However, the emerging evidence suggesting the importance of calcium deficiency in combination with vitamin D deficiency as a cause of nutritional rickets has changed the management of this metabolic bone condition.
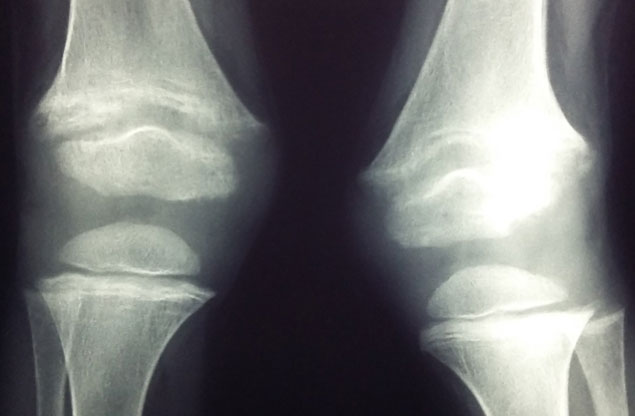
Our recent review in Bone Reports (https://doi.org/10.1016/j.bonr.2018.01.005) addressed the following key question on nutritional rickets: “Is it calcium or vitamin D deficiency (or both) that play the major role in the pathogenesis of the disease?” The case presentation in this review highlighted the importance of this question by describing a 4-year old black African boy from Johannesburg, South Africa (latitude 26° S) with clinical, radiological and biochemical evidence of nutritional rickets. The patient had a change in his walking pattern over the previous year and the parents had noted deformities of the lower limbs developing during the third year of life. He was from a low socioeconomic background and spent most of his time indoors. The infant received vitamin D fortified formula feeds up to 6 months of age. On ceasing formula feeds, his total dietary calcium intake was estimated to be <200mg/d. He was stunted and had a valgus deformity of the knees, but no other obvious clinical features of rickets. The Thacher rickets severity score was mild and his biochemical findings were suggestive of calciopenic rickets with raised PTH and 1,25 dihydroxyvitamin D (1,25(OH)2D) levels and a low 25 hydroxyvitamin D (25(OH)D) concentration. The patient was commenced on vitamin D and calcium carbonate therapy.
This review emphasises that “a combination of associated risk factors resulting in both vitamin D and dietary calcium deficiency can be accountable for the presentation of nutritional rickets in children residing in different countries worldwide with diverse cultural backgrounds”.
In this case presentation, the salient and characteristic biochemical feature that is indicative of calcium deficiency rather than vitamin D deficiency is the marked elevation of 1,25(OH)2D found prior to treatment. Thacher and Abrams (https://doi.org/10.1111/j.1753-4887.2010.00338.x) suggest that an increase in 1,25(OH)2D on the commencement of treating calcium deficiency rickets with vitamin D implies that the vitamin D status of the patient is not optimal, despite already having elevated baseline 1,25(OH)2D concentrations. This response was evident in our case as the 1,25(OH)2D concentrations increased on vitamin D and calcium therapy. Parathyroid hormone is generally increased in both vitamin D and calcium deficiency rickets. The increased PTH levels in vitamin D deficiency rickets are due to the direct effects of reduced 25(OH)D production and the subsequent decrease in 1,25(OH)2D concentrations, reducing intestinal calcium absorption and serum calcium concentrations. In calcium deficiency rickets, the inadequate absorption of calcium from the gastrointestinal tract results in an increase in PTH levels that causes an increase in the 1α hydroxylase activity thus increasing levels of 1,25(OH)2D; improving the fractional absorption of calcium.
We concluded that the important biochemical clues to underlying dietary calcium deficiency will be a low serum calcium, high 1,25(OH)2D and concomitant low-normal vitamin D status, whereas untreated vitamin D deficiency rickets will be associated with deficient 25(OH)D levels (generally <25nmol/L). Thus, it is highly recommended that the global consensus recommendations for the management and treatment of nutritional rickets especially in resource-constrained settings and in at-risk populations be followed; which entails an intake of at least 500mg of calcium per day and age related doses of vitamin D therapy (https://doi.org/10.1210/jc.2015-2175).
This case report and review of the literature on nutritional rickets was published in Bone Reports and the article was entitled “The roles of vitamin D and dietary calcium in nutritional rickets“ (https://doi.org/10.1016/j.bonr.2018.01.005). We, the authors, are Kebashni Thandrayen and John M Pettifor from Department of Paediatrics, Chris Hani Baragwanath Academic hospital and the Faculty of Health Sciences, University of the Witwatersrand; and we were invited to write the review thus no funding was required. We have no conflict of interest to declare.

Kebashni Thandrayen, MD
University of the Witwatersrand, South Africa.